Our expertise in bladder cancer
Urinary bladder cancer is the 10th most common cancer in Europe, affecting men three times more often than women.
At University Hospital Basel, specialists from urology, radiation oncology, oncology and various other disciplines work closely together to provide patients with uncomplicated access to highly qualified diagnostics and optimal treatment for bladder cancer.
Find out more about our expertise here.
Facts and figures
>1000
patients assessed and treated at the Urological Tumor Center on an interdisciplinary basis / year
>360
Patient cases with tumors in the renal pelvis, ureter and bladder discussed at the tumor board / year
30-40
robot-assisted urinary bladder removals / year
>500
Remedy applications in the urinary bladder / year
Our range of services
Comprehensive diagnostics and research
The most modern image diagnostics available.
Identification of the cancer genes and proteins that control uncontrolled tumor growth and which are potential therapeutic targets.
Continuous further development of diagnostics and therapy in the laboratory.
Specialized tumour aftercare.
Support from a multidisciplinary team
Interdisciplinary consultation hours with specialists in urology, radiation oncology and oncology.
Extensive experience in advanced bladder tumor therapy.
Innovative therapies through our active participation in national and international clinical research studies.
State-of-the-art surgery
Leading university center for oncological-robotic therapy of the urinary tract.
Endoscopic removal of urinary bladder tumors (TUR-B) and removal of the urinary bladder (cystectomy) with optimized urinary diversion and bladder-preserving therapies.
Specialized center for radical removal of the entire bladder using the DaVinci system.
Unser Team


PD Dr. Jan Ebbing
Leitender Arzt
Urologie
Teamleiter Robotische Chirurgie der Harnblase


Our specialists provide insights into their areas of expertise
Imaging: MRI of the urinary bladder
Multi-parametric magnetic resonance imaging (MRI) of the bladder provides us with detailed information about the location and extent of bladder tumors.

Example of a multiparametric MRI of the urinary bladder. Different sequences show the local extension of a bladder carcinoma on the right bladder roof.
An MRI helps us with this
An MRI of the bladder allows us to assess the size of the tumor, the depth of infiltration into the bladder wall and surrounding tissue, and the presence of lymph node metastases. This imaging supports doctors in staging and selecting suitable treatment options.
In addition, MRI can be used in long-term follow-up after treatment has been completed for the early detection of relapses or metastases.
Prof. D. Boll, Deputy Head of Radiology and Nuclear Medicine
Application of remedies in the urinary bladder
If you need bladder irrigation for bladder cancer, our experienced and trained team will be happy to help you. Thanks to our expertise in this form of therapy and the wide range of treatment options, we treat patients from all over Switzerland and nearby countries at our center.
You will receive a medically approved treatment plan in accordance with the guidelines of the European Society of Urology. Your individual appointment requests will of course be taken into account as far as possible.
Your bladder irrigations are administered via a urethral catheter in a specially created treatment lane. We make sure that the treatment is as pain-free and side-effect-free as possible.
Our specially trained staff are on hand to support you during and after your treatment.
Prof. C. Rentsch, Head Physician Urology
Heike Püschel, Head Study Nurse Urology
What our patients say
" ... today (hopefully) marks the end of a program that you can easily do without. But if such treatment is necessary, a patient can be grateful to meet competent and friendly people. From the very first day, you managed this with aplomb and allayed my fears.
In this respect, what a miracle, we live in a progressive time, which thanks to medicine extends life enormously. For this reason, as well as for the entire treatment, I would like to say a big thank you! "
Lothar Thomma, September 2023

Immunotherapy with BCG instillations
Illustration created with BioRender.com

Intravesical chemotherapy instillations
Illustration created with BioRender.com
Robot-assisted urinary bladder removal
The Urology Clinic at the USB is one of the few clinics in Switzerland that performs minimally invasive and robot-assisted bladder removal for advanced (muscle-invasive) bladder cancer.
The DaVinci® system from Intuitive Surgical™ is also used at the USB.
©2023 Intuitive Surgical Operations, Inc.
Advantages of robotic surgery
Robotic cystectomy (bladder removal) with intracorporeal urinary diversion is a state-of-the-art surgical approach that offers several advantages for patients with bladder cancer. This minimally invasive technique uses robotic technology to remove the bladder. Intracorporeal means that the urinary diversion (urinary stoma or neobladder) does not require a large open abdominal incision, but is also performed using robot-assisted keyhole surgery. The robot-assisted procedure is associated with the following scientifically proven advantages, among others.
- Faster recovery and shorter hospital stays compared to open surgery.
- Reduced post-operative pain and improved quality of life.
- Reduced risk of bleeding and less need for blood transfusions.
- More precise removal of malignant tissue and improved visualization during surgery.
- Comparable oncological results to conventional open surgery, underlining the effectiveness of this procedure.
At the USB, in addition to the conventional urinary stoma (ileum conduit), the much more complex form of urinary diversion using an orthotopic ileum neobladder is also performed completely intracorporeally (see definition above) with the DaVinci® robot. This highly complex form of urinary diversion is only performed minimally invasively in very few centers with proven experience in robot-assisted surgery.
Our robotic surgeons have proven expertise in this field and have been trained at the renowned Karolinska University Hospital in Stockholm, Sweden, one of the world's best-known pioneer hospitals for robot-assisted cystectomy.
PD Dr. Jan Ebbing, Head Physician Urology
Radiotherapy and chemotherapy as an alternative to radical removal of the bladder
In the case of a tumor that has already grown into the muscle layer of the bladder wall, a combination of radiotherapy and chemotherapy can be used as an alternative to radical removal of the bladder.
Adaptive radiotherapy of a bladder tumor. The red area shows the maximum radiation dose directed at the bladder. Green is the lower dose range, which is used to cover the lymph nodes around the bladder in order to combat any existing tumor cell nests.
The latest technology in adaptive radiotherapy
This procedure is suitable for patients whose tumors are smaller than 6 cm, have no precancerous lesions distributed on the bladder mucosa and still have good urinary flow control. The chances of success are similar to a radical removal of the bladder.
Before treatment, a cystoscopy is performed again so that as much of the tumor as possible can be removed. Subsequently, the entire bladder is irradiated every working day for 4 to 6 weeks and a concomitant, usually gentle chemotherapy is given.
At the University Hospital Basel, we use the latest adaptive radiotherapy technology. Every day, we calculate a radiation plan that is precisely adapted to the anatomy in order to optimally target the tumor and spare the healthy organs.
Dr. A. Papachristofilou, Head of the Department of Radiation Oncology
System therapies for advanced bladder cancer
In the oncology department of the USB, we offer all system therapies approved in Switzerland for bladder cancer. We strive to give our patients these therapies - wherever possible - in our outpatient clinic and thus avoid hospital stays.
In order to be able to offer innovative new concepts in addition to the approved standard therapies, we are in constant contact with national and international study groups.
These study activities have, for example, enabled us to offer an "adjuvant", i.e. supportive, immunotherapy to reduce the risk of relapse after bladder surgery several years before approval in Switzerland (Checkmate-274 study citation). None of our study patients had a relapse, and the feedback regarding this therapy was consistently positive.
The best possible therapy for your cancer
In addition to conventional chemotherapy, we also treat bladder cancer using immunotherapy and offer professional support with social and psychological issues.
Thanks to this wide range of services, we can assure our patients that we always offer state-of-the-art treatment and that we do everything we can to ensure that you receive the best possible treatment for your cancer.
Our offer also includes second opinions, for which you are welcome to register via the oncology office, for example in order to better understand your illness and the therapy concepts proposed to you.
Prof. F. Stenner, Deputy Head of Oncology
Registration for a second medical opinion:
Tel. +41 61 265 50 74
Tel. +41 61 265 50 59
or by e-mail onkologie@usb.ch
Molecular diagnostics: examination of cancer genes
An experienced team of pathology specialists assess urine cytology, tissue biopsies and surgical specimens.
In addition to a precise diagnosis of urinary tract tumors, biomarkers are determined on the tissue and cell material for the most tailored treatment possible using immunotherapy and targeted medication.
Prof. L. Bubendorf, Head Physician Pathology
Studies: Testing bladder cancer tissue in the laboratory
In order to better understand the biology of the disease, we allow the bladder cancer tissue to live on in the laboratory and can thus observe how cancer cells develop. This gives us the opportunity to test various drugs that can be used in patients.

Generation of organoids derived from cancer samples of bladder cancer patients.
Illustration created with BioRender.com
Our team is researching new ways to personalize the treatment of bladder cancer
In previous therapeutic approaches, patients with a certain type of cancer usually receive a similar treatment. However, it is becoming increasingly clear that this 'one-size-fits-all' approach is not always successful, and that while certain treatments work well for some patients, they do not show effective results for others.
To better understand the biology of the disease and personalize cancer treatment, we aim to keep bladder cancer tissue alive in the laboratory. These three-dimensional small cell clusters resemble 'mini' tumors of the respective patient. We also call these tumor cell clusters 'organoids'. These organoids serve as models or avatars to help us understand how cancer cells grow and develop, and to test different drugs that could then be used in patients. Overall, our research will ultimately help to find ways to improve and personalize the treatment of patients with bladder cancer.
Dr. C. Le Magnen, Research Group Leader Urology, Pathology
Invasion assay with patient-derived organoid of sarcomatoid urethelial carcinoma (treated with DMSO, dimethyl sulfoxide).
These lab-grown organoids show us how cancer cells grow and develop.
Invasion assay with patient-derived organoid of sarcomatoid urethelial carcinoma (treated with dexamethasone, a steroid).
The growth of tumor organoids is prevented by treatment with glucocorticoids.
Interviews: what patients tell us
We focus on the right choice of therapy and joint decision-making to maintain the best possible quality of life.
Read here what two of our patients had to say about their experiences with bladder cancer and their treatment at the USB.
'Open conversations are important and help to deal with the illness'
Patient interview on the topic of the neobladder.
The interview was conducted by Anaïs Schlenker, December 2023
How did you realize that something was wrong? What symptoms did you experience?
Without warning, I suddenly had blood in my urine. Lots of blood and every time I urinated. I had no pain, but it was a shock. That was in May 2021.
What was the path to diagnosis like?
I had my first appointment with my GP and was then referred to a urologist. The ultrasound was immediately followed by the diagnosis: several tumors.
I was called in three times for tumor removal in Liestal, where a transurethral resection of the bladder tumor was performed each time.
When the samples were taken, it was discovered that the tumor had already attacked the muscle tissue; as a result, further treatment options were discussed at an interdisciplinary tumor conference consisting of urologists, oncologists, radiotherapists and radiologists.
What treatment options were discussed with you at the University Hospital Basel?
I had my first appointment with PD Dr. Jan Ebbing at the Department of Urology at the University Hospital Basel (USB) in August 2021, accompanied by my wife.
It was explained to us that, in addition to chemotherapy, a complete removal of the bladder was necessary as the tumor had already grown into the muscles of the bladder.
Dr. Ebbing also discussed the various forms of urinary diversion with us (urinary stoma versus neobladder). The necessary requirements, the options for urinary diversion and the associated surgical risks were discussed with us.
I opted for the neoplasia and it was decided that I would first undergo chemotherapy in order to be able to treat the tumor even better.
I was able to receive the chemotherapy in Liestal, a total of four cycles. After the first cycle I still felt quite well, but after the second cycle I was struggling with skin rashes and exhaustion. And I was constantly cold. The freezing has remained and I still go to bed very early at night.
The neobladder surgery was performed successfully and without complications here at the USB by PD Dr. Jan Ebbing and Dr. Abolfazl Hosseini in January 2022.
The indication for chemotherapy is always individualized and patient- and tumor-specific. Side effects of chemotherapy do occur and are discussed with the patient by the treating oncologists during the pre-treatment consultation (editor's note).
How did you cope mentally with the diagnosis? Who is supporting you?
A diagnosis like this turns everything upside down at first; you are insecure and scared. But my family, my daughters, had more difficulty accepting the diagnosis.
However, the most valuable and important thing is the support at home. I was informed about existing external support services, but didn't want to make use of them; I'm coping well.
At the USB, all tumor patients are psycho-oncologically evaluated and, if desired, supported (editor's note).
How did you feel after the bladder removal?
The pain was severe, but I'm good with pain. I was able to endure it. Mentally, you feel insecure and I also felt somehow at the mercy of others.
Pain can occur after bladder removal surgery, but there is good pain management. The minimally invasive approach and the use of robot-assisted keyhole surgery in particular significantly reduce the trauma to the body, which is associated with faster patient recovery and fewer complications (editor's note).
Later, after the bladder catheter had been removed from the neobladder and the bladder filled with urine for the first time, I struggled with sleep deprivation; I had to set the alarm clock at night, first every two, then every three hours, so that there was no overloading with the new bladder. However, the accompanying pelvic floor therapy went well.
A neobladder has no sensitivity and no motor activity. The urine volume must first be trained. It is therefore normal for patients to have to empty the neobladder at night and set an alarm clock. About 30% of male patients with a neobladder remain incontinent at night (more than 1 insertion), whereas about 96-98% of male patients are dry during the day, without restrictions (editor's note).
Would you make the same decision (for a neobubble) again?
Yes, it seemed like the best option for me right from the start.
How important is it to you to trust your doctor? Do you feel that you are in good hands?
Yes, I feel well looked after here at the USB.
How are you feeling today? Are there any restrictions in your everyday life?
I was able to return to work in May 2022. Everything works well during the day and I have no problems or complications. At night (when my head isn't thinking) I have to wear insoles. I no longer have to take any medication. With the exception of erection support.
What happens next?
I am called in for a check-up every six months and then once a year. So far, everything has been normal.
What would you like to give other patients?
Communicating openly with family and friends. I felt the need to spare my loved ones and family, but open conversations were the best way to help everyone deal with the illness.
Even with work colleagues and acquaintances, there were those who avoided me and those who asked directly how I was doing. I was able to give a direct answer, and that was always really good and helped me to deal with the situation.
'I want to show my body that I'm not giving up'
Patient interview on the topic of bladder tumors and instillation.
The interview was conducted by Anaïs Schlenker, December 2023
How did you realize that something was wrong? What symptoms did you experience?
It all started with a sore hip in the fall of 2022, when I was in the USA on business. I came back to Switzerland and had to undergo hip surgery in December. Following the operation, blood was found in my urine, a typical symptom of bladder cancer.
What was it like to be diagnosed and how did you feel after the operation?
The diagnosis after the CT confirmed the suspicion: a bladder tumor. I was then unable to return to the USA and regular work is still not possible. However, this is only partly due to the bladder tumor and the associated therapy. I am also struggling with the consequences of reactive arthritis in my knee and my operated hip.
I had surgery at St. Claraspital in January 2023. The first TUR-B (transurethral resection of bladder tissue) was followed by a resection.
BCG (Bacillus Calmette-Guérin) instillation was started in March. After the third instillation, my knee and calf swelled up. A side effect of the instillation that was not recognized as such. This was followed by an operation on my knee and a puncture in my hip. The treatment had to be discontinued.
At the end of May, three small tumors were discovered during a cystoscopy. Two tumors were superficial, one tumor turned out to be a carcinoma in situ (CIS) with a high risk of recurrence.
To date, the findings are: no more visible tumors.
How are you coping mentally with the diagnosis? Who is supporting you?
This marathon of doctors and diagnoses is extremely stressful and tiring. My daughter accompanied me to the appointments a few times. Of course, you also try to gather information yourself through all available channels.
I also sought external psychological help from time to time. But only for a short time. Ultimately, you have to deal with the illness on your own. I also try not to burden my family too much with it.
I also had to learn that the emotional life during such treatment is not so easy to explain and that you shouldn't underestimate the psychological strain.
When were you referred to the USB?
After the second TUR-B, I received a first instillation of epirubicin at St. Claraspital. This is the standard treatment.
In August 2023, a referral to the USB was discussed at the tumor board with Prof. Cyrill Rentsch. A docetaxel/gemcitabine combination therapy is offered here at the Urology Clinic, which is more promising. The therapy was then started immediately.
How often do you come to our clinic?
The procedure for the instillation cycle is as follows: for six weeks I received alternating doses of chemotherapy flushed into the bladder on two consecutive days.
On the first day a dose of Docetaxel, on the following day a dose of Gemcitabine. This was followed by a four-week break. Maintenance therapy was then started after a positive cystoscopy.
The first consultation is held after the consultation appointment for the last round of instillations. The patient appears athletic, open, composed, but also tired. This is one of the side effects that he struggles with in the first 3-5 days after instillation. Exhaustion and nightmares also bother him.
Do you feel you are in good hands with us?
After my hospital stays and visits to doctors at St. Claraspital and Merian Iselin Spital, I had to readjust to the USB. The USB is a big place, so you can feel like one of many. But the priority is to get the right treatment. This is the case here.
I feel that I am in good hands with my attending physician, Prof. Cyrill Rentsch. My thanks also go to Heike Püschel, Study Nurse, who looks after me with great empathy during every examination. This is extremely valuable.
What happens now?
I am currently undergoing maintenance treatment. For 12 months, I come to the urology clinic every month on two consecutive days and receive a dose of Docetaxel on the first day and a dose of Gemcitabine on the second day.
What would you like to give other patients?
For me, it's important to feel my body and keep moving. In my case, swimming and running training sessions helped me a lot to forget about the tumor, at least temporarily.
That's what I would say to someone living with a similar diagnosis - don't let up, fight. And believe in yourself.
Brochures for patients on the subject of bladder cancer
'We recommend the information brochures 'Bladder cancer' and 'The urostomy' from the Swiss Cancer League. There you will find further useful information on the subject.

Frequently asked questions

What triggers bladder cancer?
The main risk factor for bladder cancer is smoking. Stopping smoking can have a positive effect on the relapse and progression of bladder cancer. Read more about our stop smoking consultation at the USB.
What are the symptoms?
Signs include pain when urinating and frequent urination. However, the main symptom is visible or non-visible, painless blood loss in the urine. Patients with these symptoms should definitely be seen by a urologist.
Verdacht auf Blasenkrebs - Wie geht es weiter?
Besteht der Verdacht auf Blasenkrebs werden wir eine Blasenspiegelung durchführen. Heutzutage kann dieser Eingriff durch den Einsatz einer flexiblen Kamera ambulant und ohne Narkose schmerzfrei in der Sprechstunde durchgeführt werden. Eine Blasenspiegelung dauert lediglich wenige Minuten. Zusätzlich werden wir eine Blasenspülung durchführen und so untersuchen, ob bösartige Blasenschleimhautzellen gefunden werden können. Zeigen sich in diesen Untersuchungen Auffälligkeiten, wird kurzstationär eine Gewebeprobe aus der Blase, minimalinvasiv ohne Hautschnitt, durch die Harnröhre hindurch entnommen.
What forms of therapy are available?
If a bladder tumor is found in the cystoscopy, it is removed through the urethra under anaesthetic. When first diagnosed, most bladder tumors are limited to the mucous membrane (70%) and the bladder can be preserved.
Urinary bladder tumors limited to the mucous membrane have a high risk of recurrence. To reduce this risk, after removal of the tumors, medication is injected into the bladder via the urethra at regular intervals using a catheter to reduce the risk of recurrence. Read more about our instillation therapy.
If the cancer has already grown into the muscles of the bladder when it is first diagnosed, the bladder must be surgically removed or treated with radiotherapy and chemotherapy.
Read more about robot-assisted cystectomy, radiotherapy and chemotherapy.
Rarely, however, bladder cancer has already spread throughout the body. In this case, cure by surgery and radiotherapy is no longer likely. However, there are good therapies that can greatly prevent further progression of the disease.
What are the chances of recovery?
The earlier bladder cancer is detected, the higher the chances of recovery. If the tumor has not yet grown into the muscle layer of the bladder, the chances of recovery are around 80%.
Does bladder cancer often return?
Unfortunately, non-muscle-invasive bladder cancer often returns even after complete removal.
We offer our patients individual tumor follow-up care to detect bladder tumor recurrences at an early stage and treat them accordingly.
Our clinic also has extensive experience in advanced bladder tumor therapy.
Approach & Contact
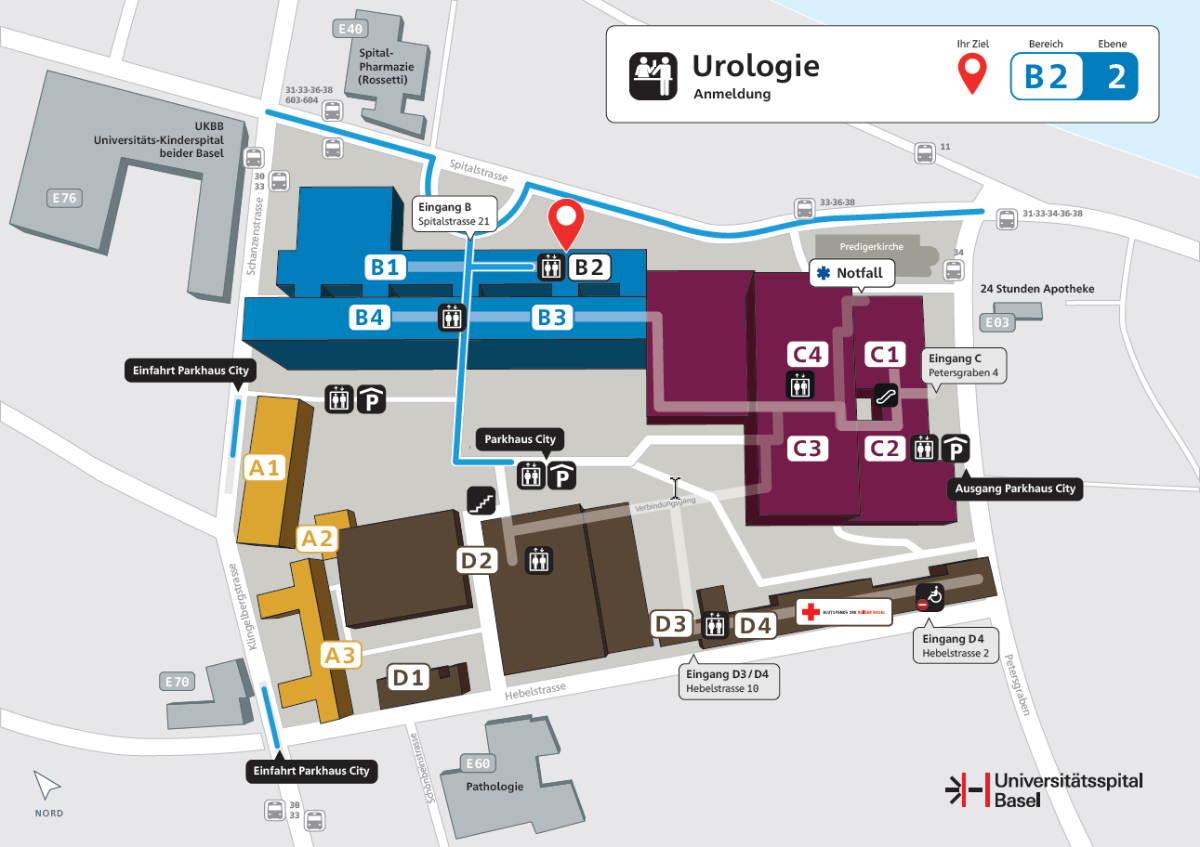
Address
|
University Hospital Basel |
By streetcar
| Take streetcar line 11 to the University Hospital station and then follow Spitalstrasse on foot for about 250m to the entrance. |
By car
| Please use the parking garage City, entrance Schanzenstrasse or Klingelbergstrasse. |
Contact us
Urology registration office
Availability: Mon-Fri, 08.00 - 16.00 hrs
Phone +41 61 265 72 80
anmeldung.urologie@usb.ch
Contact for emergencies
During operating hours, please contact the Urology Registration Office. For urological emergencies outside of operating hours, the Emergency Center at the USB is there for you around the clock:
Emergency Center University Hospital Basel
Petersgraben 2
4031 Basel
Phone +41 61 265 25 25
Contact for queries about your operation
Surgery Coordination Urology
Phone +41 61 328 58 15
op.urologie@usb.ch
Contact for consultation appointments at Felix Platter Hospital
Registration office Urology UAFP
Urology consultation hours on Mon and Fri, all day from 8.00-16.30 and Tuesday afternoon from 13.00-16.30
Phone +41 61 326 42 10
urologie.uafp@usb.ch
Contact applications
chefarztsekretariat.urologie@usb.ch
Phone +41 61 328 72 84


