Delirium management care program
Acute confusion, also known as delirium, manifests itself as a change in the patient's behavior from one day to the next.
Relatives often report that they do not know the person like this. Perception, recognition, thinking, awareness and actions are altered for days. The altered behavior usually regresses.
Delirium can occur at any age. Older people (especially those with many concomitant illnesses or dementia) are particularly susceptible. The severity of the acute illness also influences the development of delirium.
For example, delirium is a common complication in patients in intensive care units. Delirium is often a burden for patients and their relatives and can have many negative consequences.
Delirium requires rapid and expert treatment.
Offer
The Delirium Management Nursing program is responsible for the hospital-wide implementation of the nursing delirium treatment standard at the USB.
This includes the nursing delirium consultation service, which works closely with the interprofessional acute geriatric consultation service to support the treatment teams at the USB in the diagnosis and treatment of patients with delirium.
In addition, the Delirium Management program offers a comprehensive range of further education and training courses for USB employees as well as interested external parties.
Program management

Kevin Seiler
Programmleiter Delirmanagement
Abt. Praxisentwicklung und Forschung Pflege
Tel. +41 61 556 56 94
Further information on delirium
Questions and answers on the subject of delirium
Information for relatives
Information for professionals
Delirium management care concept
medStandards University Hospital Basel
- Cross-hospital prevention, screening and treatment algorithm
- medStandard (emergency standard) Delirium
- medStandard (alcohol withdrawal, prophylaxis)
- medStandard (Alcohol withdrawal)
Further information
World Delirium Awareness Day 2025
On the occasion of this year's World Delirium Awareness Day 2025, we would like to show how multi-layered and complex delirium is.
We have interviewed experts from the University Hospital Basel about their experiences. One person affected also has his say and describes what delirium felt like for him.
Interview with a delirium sufferer
You are still quite young, so definitely not at an age that one would traditionally associate with delirium - can you tell us how it came about that you developed delirium?
I had just been on tour with my band in the USA. During the tour, I started to feel a bit sickly, which got worse over several days. I first tried to treat the whole thing with medication from the pharmacy - unfortunately without success. I then played a show in the evening and went straight to the hotel and took a shower afterwards. I caught legionella there, as I now know. The next day I still didn't feel any better, on the contrary, I even had blood in my stool.
So me and my bandmates decided it was time to go to hospital. When I arrived at the emergency room, I had to wait a long time, about 8 hours. The doctors' first assumption was Covid-19 with pneumonia. I was then put on infusions and had an MRI.
From that point on, my memories started to blur.
From what my colleagues and my partner told me, I know that I was in that hospital for 5 days with severe pneumonia. The next thing I remember is waking up in a hospital in Switzerland. As I know today, I was brought to Switzerland by Rega - I was in an induced coma for 13 days. My lungs failed in the meantime, which is why I was intubated.
Do you have specific memories of the delirium itself?
Yes and no, I do remember having some extreme dreams that felt extremely real to me at the time.
- In one dream, for example, I was convinced that Rega had left me on a bridge in Frankfurt.
- Or that I was on my way to Las Vegas in a private jet with rich strangers.
- Or that I was buried under cardboard in a garage and couldn't move.
I also believed, for example, that I had read something Russian on an infusion in hospital and from then on I was convinced for a night that I was Russian myself and that I was in Russia.
I was also very suspicious, for example I wanted to sue the hospital and kept asking to see the head doctor. I complained that I had been treated badly. But it all happened in my dreams and had nothing to do with reality. At that moment, however, I was unable to separate dreams from reality.
What helped you to come out of the delirium?
It was definitely my partner and my parents. My partner kept a diary the whole time, which helped me to close the gaps in my memory as well as possible. Also the nurses and doctors, who explained my situation to me again and again in a calm, very matter-of-fact tone.
What would you say is the best way to help delirium sufferers in this situation?
I think it's important to help them get back to reality and explain that what's happening is real. As the person affected, you may not yet be able to understand what has happened, but you do realize what is happening. It is certainly important that relatives and hospital staff always keep this in mind. In addition, people with delirium should not be confirmed in their dreams. Instead, an attempt should be made to explain as objectively as possible what is actually happening.
Were there any long-term effects for you after the delirium?
The whole experience has certainly changed my perspective on life to some extent - but that's a rather positive thing for me. I've been able to come to terms with what happened and fortunately I don't have any bad feelings about what I experienced.
A for Awareness
Kevin Seiler on the topic of awareness of delirium in hospital.
C for CAM
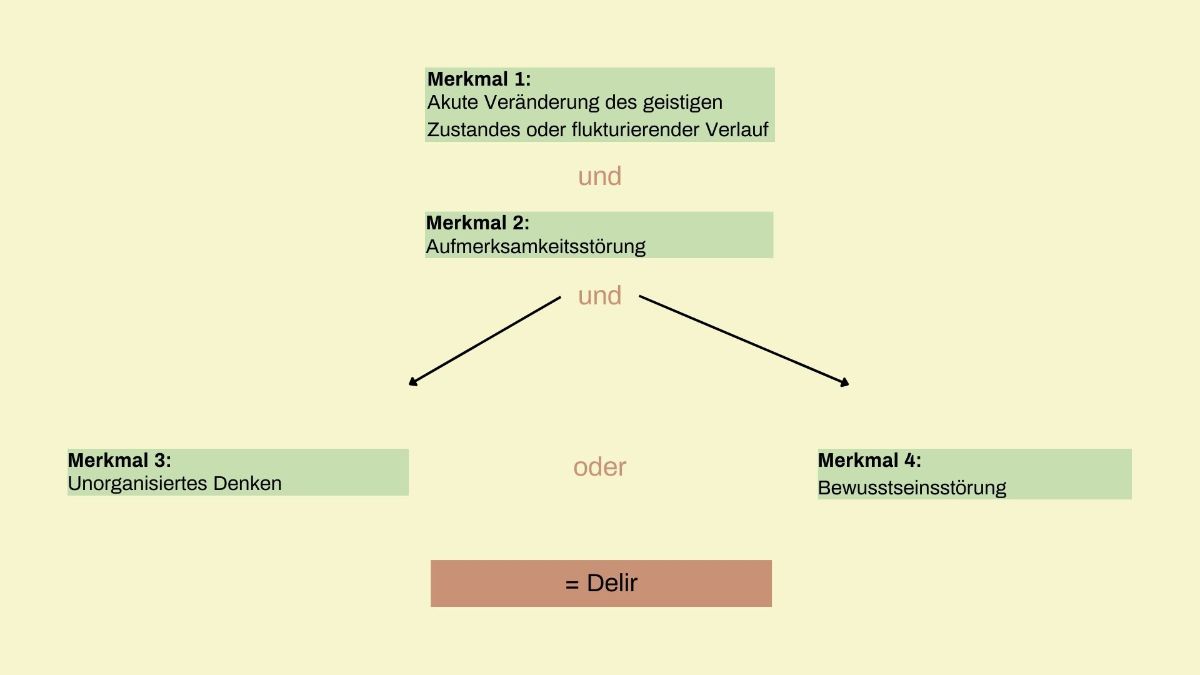
The Confusion Assessment Method (CAM) is a diagnostic algorithm consisting of four criteria. There are different versions of the CAM. At the University Hospital Basel, we use the mCAM-ED (modified Confusion Assessment Method for the Emergency Department), among others, to detect delirium.
E for detection
Thomas Dreher on the topic of detection and why early detection of delirium is so important.
G for Look and listen carefully

I like hedgehog ball
David Hueck on the hedgehog ball.
K for comfort
Thomas Dreher on working with people with delirium in an emergency setting.
M for Month backward test
Renzo Weisskopf on the subject of the Months Backward Test: A test to check attention. Attention deficit disorder is the leading symptom of delirium.
O for disorientation

People with delirium often have problems with orientation. They should therefore be mobilized and always have access to their own glasses, hearing aid, watch and other aids so that they can orient themselves better in the room and know what is happening around them.
Q for quality on USB
Kevin Seiler on the quality of delirium management at the USB.
S for voice
Katja Reichenstein on the subject of voice.
U for clock
Christian Emsden about watches.
W for World Delirium Awareness Day 2025

World Delirium Awareness Day (WDAD) is held annually in March to raise awareness of delirium and its impact on patients, families and healthcare systems. This year's WDAD is March 12, 2025.
You can find more information here: www.deliriumday.com
Y for Your turn!
We hope that our delirium alphabet has given you a better understanding of the many facets of delirium. Now it's up to you! Help us to raise awareness of delirium even further: talk to those around you about the topic, share our information content and interact with us on our social media channels(Instagram, Facebook and LinkedIn).
B for urge to move
Mauritius Reinitzer on people with delirium who have a strong urge to move and how this can be countered.
D for dementia
Katja Reichenstein on the topic of dementia and the connection to delirium.
F for family and relatives

Recognizing delirium can sometimes be difficult. This is where family and relatives can be a great help. They know best what the patient is like and can recognize unusual behaviour - and therefore an indication of delirium - more clearly.
H for stroke
Renzo Weisskopf on the topic of stroke and why it is not so easy to recognize delirium in patients after a stroke.
J for young and old

L for speech therapy
Claudia Troll on how speech therapy can help with delirium.
N for follow-up consultation
Christian Emsden on the topic of follow-up consultations at the USB.
P for care

Nursing, i.e. non-pharmacological measures, are the be-all and end-all of delirium prevention and treatment. Research shows that this is the only way to prevent, shorten and specifically treat delirium.
R for Red Threads - An experience report
Renzo Weisskopf on how a patient perceived hallucinations during his delirium.
T for handkerchiefs
Mauritius Reinitzer on handkerchiefs.
V for behavior
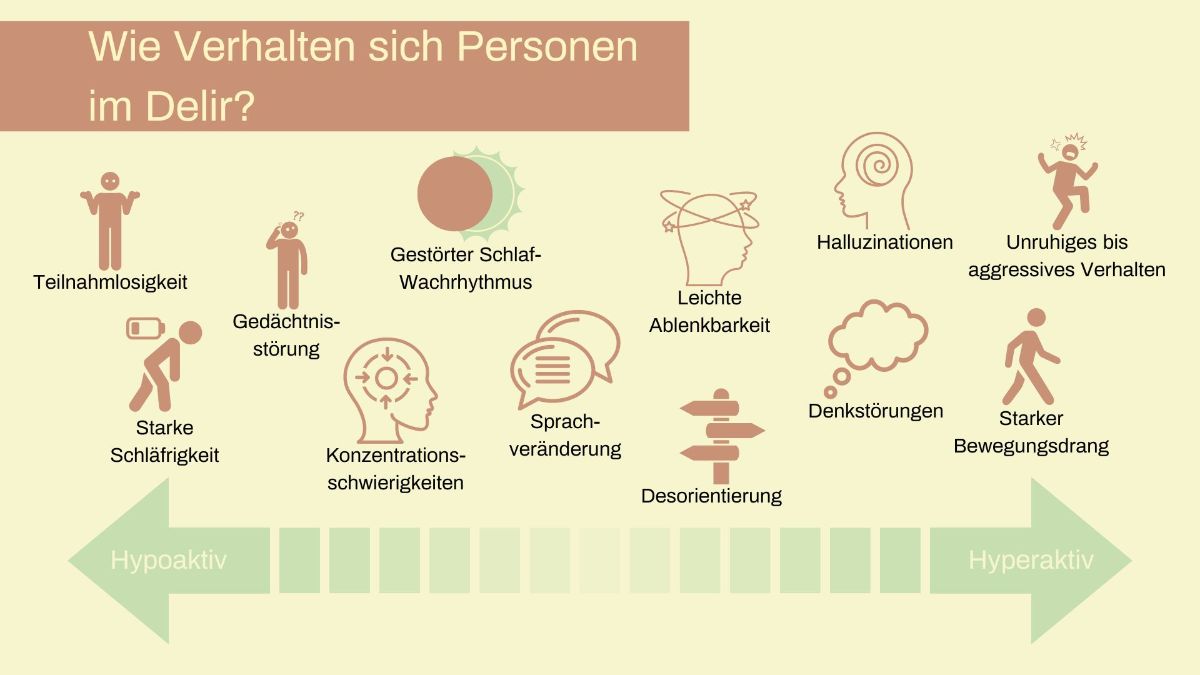
The symptoms of delirium can look very different. For example, some people behave very calmly (hypoactive), while others have a strong urge to move (hyperactive).
X like the search for the unknown
As with the "perfect crime", delirium can present complex "cases". In our hospital, however, it is not the police or detectives who solve the cases, but the nurses, doctors and therapists who shed light on the darkness and clarify and treat the usually multifactorial causes of delirium.
A joint, interprofessional approach is key.
Z for lemon sorbet
Claudia Troll on lemon sorbet.
Further education and training
Introduction to delirium management for HF/FH nurses, healthcare assistants and ZTPs
- February 6, 2026, 8.30-16.30
- April 17, 2026, 8.30-16.30
- August 28, 2026, 8.30-16.30
- November 27, 2026, 8.30-16.30
5 day course Dealing with (acute) confusion
October 26 - 30, 2026, 8:30 a.m. - 5:30 p.m.
Resource group meeting
- Tuesday, February 24, 2026, 4.00-5.00 p.m.
- Tuesday, April 14, 2026, 4.00-5.00 p.m.
- Tuesday, June 23, 2026, 4 p.m.-5 p.m.
- Tuesday, August 18, 2026, 4:00 p.m. - 5:00 p.m.
- Tuesday, October 6, 2026, 4:00 p.m. - 5:00 p.m.
- Tuesday, December 1, 2026, 4 p.m.-5 p.m.
Location: Large meeting room, Hebelstrasse 36, 1st floor.
Registration by e-mail to Kevin Seiler Program Manager Delir Management
Workshop Dementia Delirium Resource Group
September 11, 2026, 8:30 a.m. - 4:30 p.m.
September 25, 2026, 8:30 a.m. - 4:30 p.m.
