Brain Tumor Center
Welcome to the Brain Tumor Center of the University Hospital Basel
We specialize in the comprehensive diagnosis and treatment of brain tumours. Our aim is to support patients and their families quickly, competently and sensitively - from the first suspicion to treatment and aftercare.
"Reliable, cutting-edge medicine for our patients: That is our daily claim, which is confirmed by repeated certifications."


PD Dr. Dominik Cordier, Head of the Brain Tumor Center
Our offer
More than medicine
In addition to state-of-the-art diagnostics and therapy, we attach great importance to holistic support. This includes psychological support, physiotherapy, ergo- and speech therapy as well as close support with dedicated contact persons throughout the course of the illness.
Interdisciplinary cooperation
for your best possible treatment.
Specialists from neurosurgery, neurology, oncology, radiotherapy, radiology, pathology and other disciplines work closely together.
All findings are discussed promptly in a joint tumor board in order to develop an individually tailored treatment concept.
Disease patterns

We treat all forms of tumor diseases of the nervous system. Because every disease is individual, we develop a customized treatment concept for each patient.
Frequently occurring diseases are
Brain metastases
metastases of other cancers in the brain.
Meningiomas
Mostly benign tumors of the meninges, often surgically treatable.
Gliomas
Malignant tumors of the supporting cells of the brain, slow to aggressive growth.
Rare tumors
In addition to the 3 most common tumors, there are >120 other, rarer tumor types
Diagnostics
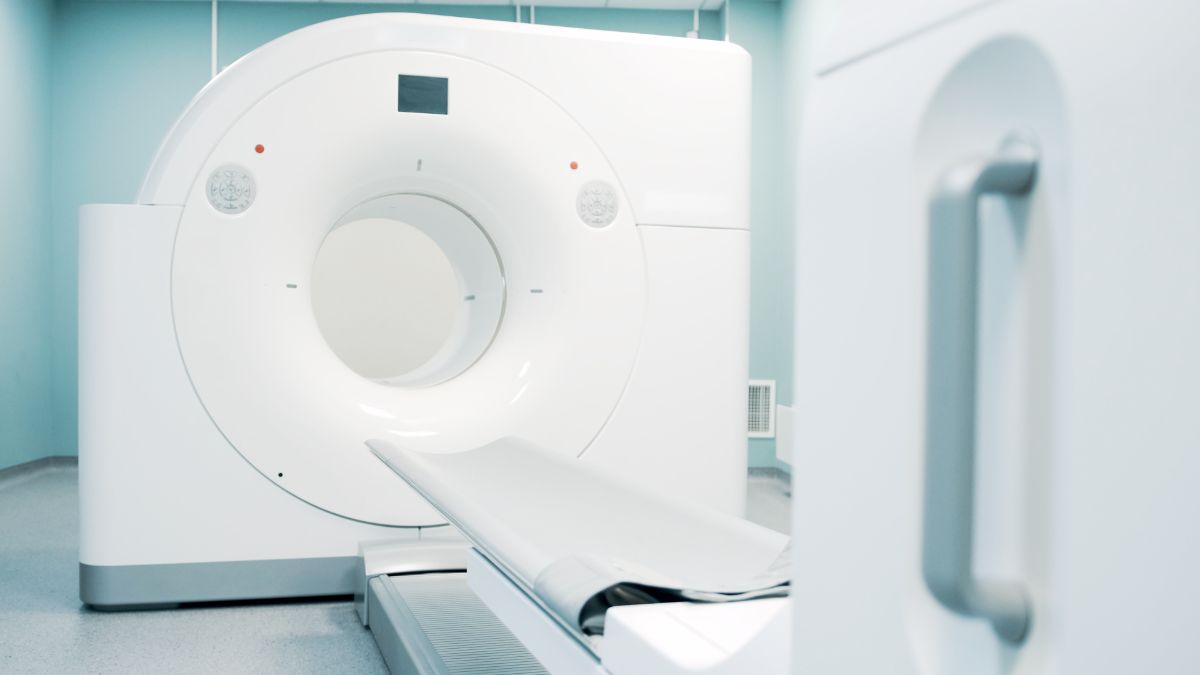
The most important examination when a brain tumor is suspected is magnetic resonance imaging (MRI or MRT). In addition to the standard images, special procedures such as perfusion MRI, MR spectroscopy or FET-PET/CT can provide additional information about the type of tumor.
"Even the most modern diagnostic CT and MRI procedures can be used to narrow down the basic characteristics of a possible tumor disease, which is crucial for further diagnostic confirmation and treatment"
Dr. Johanna Lieb
If there is a strong suspicion, tissue is obtained - either directly as part of an operation to remove the tumor or initially by means of a biopsy to confirm the diagnosis.
Only the fine tissue analysis allows a clear classification and is decisive for the planning of further therapy.
"State-of-the-art analysis methods, which were co-developed at the University Hospital Basel, allow ultra-fast and highly precise brain tumor diagnostics - often within 24 hours of the operation. This provides our patients with rapid certainty in a stressful situation and enables treatment to be planned without delay."
Prof. Stephan Frank
Unfortunately, a diagnosis using blood tests is not yet possible, but is the subject of active research at the University Hospital.
Treatment

Operation
Surgery has two main objectives: to remove the tumor as completely as possible and at the same time to maintain normal brain function. In the case of benign tumors, permanent recovery is often possible after complete removal. In the case of malignant tumors such as glioblastoma, removing as much of the tumor as possible improves the prognosis and survival time.
The absolute priority is to preserve function. If necessary, a small residual tumor is deliberately left to avoid permanent neurological damage. Such remnants can be monitored for years or treated with radiotherapy or medication.
To increase the safety of the operation, we use state-of-the-art procedures: intraoperative navigation, fluorescence techniques, ultrasound, functional monitoring and awake operations to monitor speech, movement and vision. In this way, tumors can be removed with particular precision while important functions are spared.
The operation is usually followed by a short inpatient stay of often less than a week. If necessary, this is followed by inpatient or outpatient rehabilitation, e.g. with physiotherapy, occupational therapy, speech therapy or psychosocial support.
The next steps depend on the type of tumor:
-
Benign tumors usually only require regular follow-up MRI scans.
-
Malignant tumors are usually followed by additional therapies such as radiotherapy and/or systemic therapies
"Our interdisciplinary team helps patients to regain their mobility and independence quickly and in the best possible way after surgery."
Emöke Wellinger
Radiotherapy
Radiotherapy is an important complement to surgery and is used in particular for high-grade brain tumors and brain metastases. The aim is to specifically destroy remaining tumor cells and slow down tumor growth in the long term. We use high-precision linear accelerators at our sites in Liestal and at the University Hospital Basel for this purpose.
In selected cases, we also work closely with the Paul Scherrer Institute (PSI). State-of-the-art procedures such as proton irradiation are available there, which can be particularly suitable for certain types of tumors or sensitive localizations.
Radiosurgery - a single or few high-dose, highly focused radiotherapy sessions - is also a gentle alternative to surgery for small, clearly defined tumors.
"Our aim is to achieve effective tumor control using the latest radiation techniques while sparing healthy tissue as much as possible."
PD Dr. Markus Gross
Drug therapies
Drug therapies, which can complement surgery and radiotherapy, also play an important role in the treatment of brain tumors:
-
In the case of brain metastases, the therapy often depends on the original cancer (e.g. lung, breast or skin cancer) and can vary greatly: from chemotherapy to targeted drugs to immunotherapies.
-
For high-grade gliomas, tablet therapy with temozolomide is generally used, usually in combination with radiotherapy. In certain situations, other drugs such as lomustine are also used.
-
In selected cases, new targeted substances (e.g. vorasidenib) or trial treatments can also be offered.
Our patients are supported by the medical oncology team throughout the entire systemic therapy. There are dedicated contact persons who not only manage the treatment, but also provide close advice and support.
"Successful systemic therapy requires not only the right medication, but also continuous support - that's why we stand by our patients' side."
Dr. Benjamin Thiele
Epilepsy
Many patients with brain tumors develop epileptic seizures during the course of the disease. These occur when tumor tissue or scars disrupt the electrical balance in the brain. In most cases, epilepsies can now be treated well with medication (antiepileptic drugs). Careful adjustment is important, as each drug can have different side effects - such as tiredness, difficulty concentrating or interactions with other medications.
After a seizure, a temporary driving ban usually applies to ensure your own safety and that of others. Professional or private activities may also be temporarily restricted.
"We research and develop new diagnostic and therapeutic strategies to improve the care of brain tumor patients. We also deal with the neurological consequences of brain tumors such as epileptic seizures, cognitive deficits and paralysis"
PD Dr. Martin Diebold
Rehabilitation and aftercare
After an operation, rehabilitation can help to regain lost functions and get back to everyday life more quickly. Depending on requirements, physiotherapy, occupational therapy or speech therapy may be used. These therapies can be carried out either as an inpatient in a specialized rehabilitation clinic or as an outpatient close to home. We work closely with regional rehabilitation facilities.
Regular follow-up examinations and MRI checks ensure the long-term success of the treatment.
Support & guidance

Our comprehensive treatment goes beyond surgery, radiotherapy and medication. We offer holistic support that strengthens mental stability, promotes physical functions and provides security in all phases of the disease - from firm psychological support to palliative and complementary services.
We will help you to select and connect with the appropriate services - talk to your therapist at any time.
Complementary medicine
In addition to standard therapy, our cooperation partner, the Arlesheim Clinic, offers complementary medical procedures such as mistletoe therapy. We will be happy to organize a connection if you are interested.
Palliative medicine
If a cure is not possible, the focus is on quality of life and symptom control. Our palliative care offers comprehensive care, alleviates symptoms and provides empathetic support for patients and their relatives.
Nursing support
Our nursing staff support our patients throughout their stay in hospital.
With professional competence and empathetic support, they take comprehensive care of the patient's needs during this difficult life situation.
Physiotherapy, logo therapy and occupational therapy
Specialized therapies promote mobility, speech and independence. They are started during an inpatient stay and can be continued on an outpatient basis close to home. They make a decisive contribution to returning to everyday life.
Psycho-oncology
Cancer always affects mental health too. Our psycho-oncologists provide support in overcoming fears, finding sources of strength and actively shaping everyday life despite illness.
Psycho-oncology
Cancer always affects mental health too. Our psycho-oncologists provide support in overcoming fears, finding sources of strength and actively shaping everyday life despite illness.
"A tumor diagnosis can turn your life upside down - we help you deal with this burden and find new stability."


Sabrina Elia
Research & clinical studies

As a certified center for brain tumors, we combine modern patient care with basic and applied research.
In addition, we conduct clinical studies that investigate new therapies and clearly focus on the benefits for patients. In this way, we are actively trying to improve the treatment options for our patients in the future.
Please contact us if you are interested.
Under the following link and tab "Brain tumors" you will find an overview of current studies.
"We are researching new ways of targeting the immune system against brain tumors - in order to quickly translate findings into more effective therapies. Through clinical trials, we offer our patients the opportunity to actively participate in such new developments."


Prof. Gregor Hutter

Unser Team
Management


Team





Prof. Stephan Frank
Leitender Arzt und Fachbereichsleiter Neuro- und Ophthalmopathologie
Pathologie
Klinische Professur für Neuro- und Muskelpathologie, Mitglied Tumorzentrum, Neuro- und Muskelpathologie, Molekularpathologie
Tel. +41 61 328 63 90

Prof. Jörg Halter
Leitender Arzt
Hämatologie
Leitung Behandlungszentrum Stammzelltransplantation


Prof. Heinz Läubli
Leitender Arzt / Leitung Klinische Forschung
medizinische Onkologie FMH, allgemeine Innere Medizin FMH, Mitglied Tumorzentrum, Forschungsgruppenleiter Tumorimmuntherapie, DBM und DKF
Hirntumore, Hauttumore, Thoraxtumore, Immuntherapie, Krebsimmunologie


Dr. Johanna Lieb
Kaderärztin, stv. Leitung Neuroradiologie, Mitglied Tumor- und MS-Zentrum
Radiologie und Nuklearmedizin
Tel. +41 61 328 65 93

Dr. Benjamin Thiele
Oberarzt
Innere Medizin und Hämatologie und Onkologie (D), Hämatologie (FMH, CH)
ZNS Tumore, GI Tumore, Lymphome



Prof. Dr. phil. Dr. med Damian Wild
Leitung Nuklearmedizin
Radiologie und Nuklearmedizin
Radiologie und Nuklearmedizin, Zentrum für neuroendokrine und endokrine Tumore
Tel. +41 61 556 53 84
"For a prompt assessment of your case, we need a current medical report with the previous treatments, current images and ideally the pathology report."
PD Dr. Dominik Cordier
Contact us
Whether for initial clarification, ongoing treatment or to obtain a second opinion - we are here for you. Our team will take the time to answer your questions, help you make an appointment and reliably guide you through the next steps.
Office
Denise Weingartner
Phone +41 61 265 39 05
E-mail neurochirurgie@usb.ch
For referrers:
We greatly appreciate the good cooperation with you. We will therefore deal with your request promptly and can also be reached directly using the following contacts.

